The Architecture of the Second Brain: An In-Depth Scientific Analysis of the Gut-Microbiome-Brain Axis
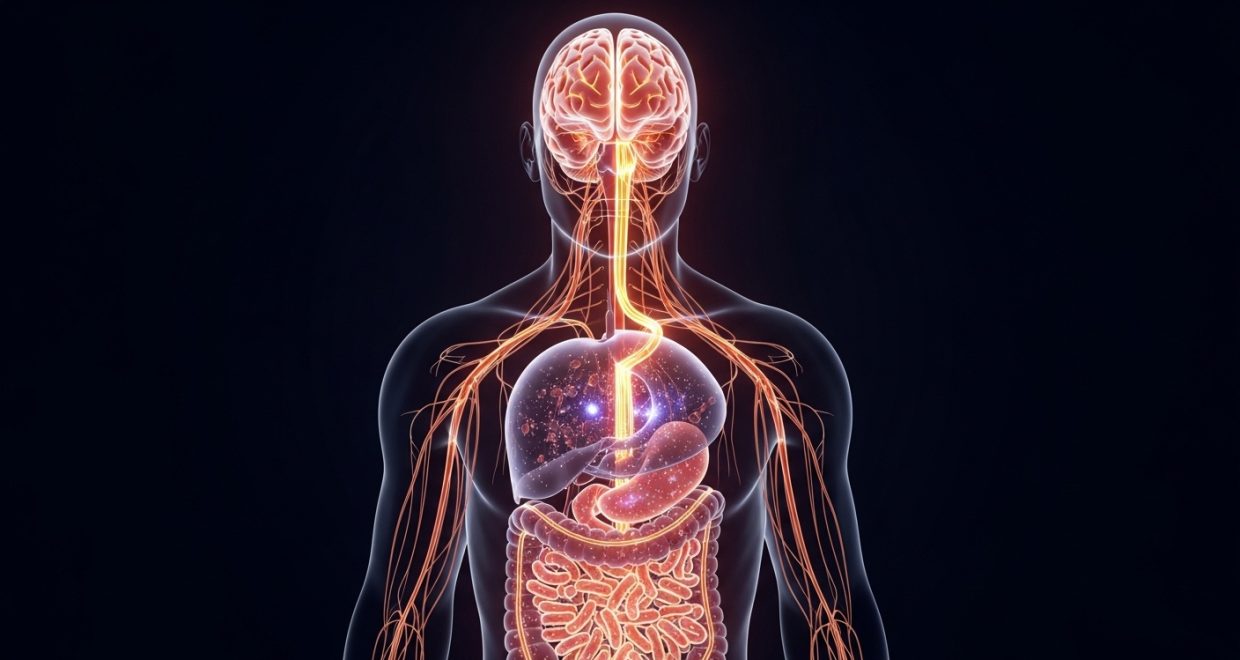
The human body is not a single entity, but a complex “holobiont”—a symbiotic collection of human cells and trillions of microbial tenants. For centuries, the medical community viewed the gastrointestinal tract as a simple biological furnace designed to extract calories. However, we have entered a new era of “Neuro-gastroenterology,” where the gut is recognized as the Enteric Nervous System (ENS), a sophisticated sensory organ and emotional regulator that functions with a level of complexity rivaling the brain in our skulls. This article provides an exhaustive examination of how this “Second Brain” and its microscopic inhabitants dictate the human experience, from the depths of our moods to the specific nature of our daily cravings.
1. The Evolutionary Origins of the Enteric Nervous System
The “Second Brain” is not a secondary evolution; in many ways, it is our first. Evolutionarily, primitive organisms developed digestive tracts and a nervous system to manage them long before they developed complex brains for abstract thought. This ancient origin is why the Enteric Nervous System (ENS) is so autonomous. It consists of a dense meshwork of neurons embedded in the lining of the esophagus, stomach, small intestine, and colon. Because it had to manage the life-sustaining process of digestion without constant oversight from the central nervous system, it evolved to be self-reflexive. This deep biological history explains why “gut feelings” often feel more primal and urgent than logical thoughts; they are rooted in the very foundation of our survival mechanisms.
2. The Vagus Nerve: The 24/7 Biological Fiber-Optic Cable
The Vagus Nerve is the primary physical conduit of the gut-brain axis, extending from the brainstem down to the abdomen. While it was long believed that the brain used this nerve to “boss” the gut around, modern tracer studies have revealed a radical 90/10 information asymmetry. Approximately 90% of the fibers in the vagus nerve are afferent, meaning they carry information upward from the gut to the brain. Your brain is essentially a passenger on a ship, receiving constant telemetry from the engine room (the gut). If the gut is inflamed or the microbiome is in a state of chaos, the vagus nerve sends a continuous stream of “error codes” to the brain, which the subcortical regions interpret as generalized anxiety, unease, or a sense of impending doom.
3. The Microbiome: The Pilot of the Second Brain
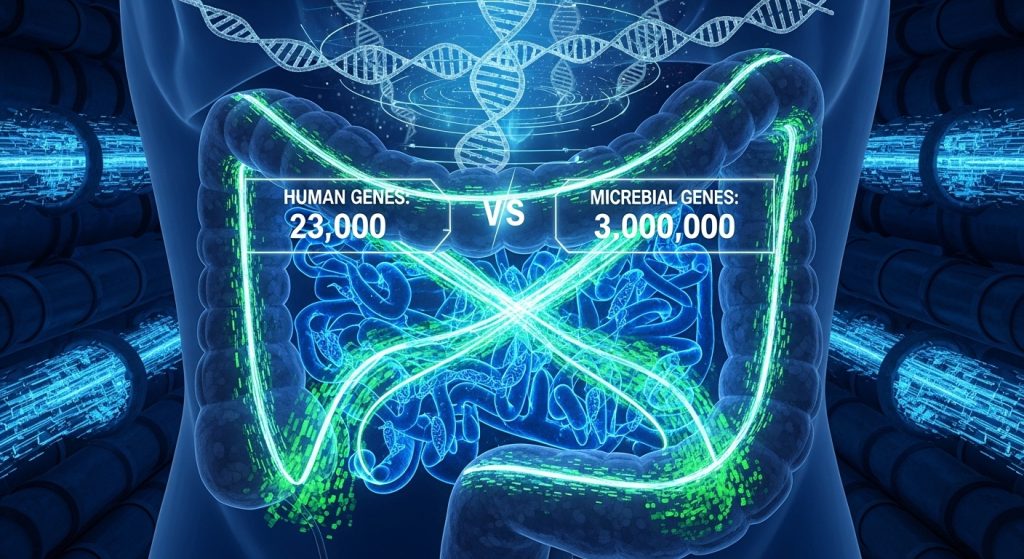
While the ENS provides the neural hardware, the microbiome—the 100 trillion bacteria, fungi, and viruses living in your gut—acts as the software. These microbes possess over 3 million unique genes, vastly outnumbering the 23,000 genes in the human genome. This genetic diversity allows microbes to perform metabolic functions that human cells cannot, such as breaking down complex fibers into Short-Chain Fatty Acids (SCFAs). These SCFAs, particularly butyrate, are not just food for gut cells; they are signaling molecules that enter the bloodstream and cross the blood-brain barrier to regulate microglia (the brain’s immune cells), effectively acting as a master dial for neuroinflammation.
4. Serotonin Synthesis: The Gut as the Body’s Primary Factory
It is a common misconception that serotonin, the “happiness molecule,” is primarily a brain chemical. In reality, roughly 95% of the body’s serotonin is produced by enterochromaffin cells in the gut. While this gut-derived serotonin does not directly cross the blood-brain barrier, it influences the brain by regulating the availability of its precursor, tryptophan. When the gut is healthy, tryptophan is converted into serotonin. However, when the gut is inflamed, the body activates the “Kynurenine Pathway,” which diverts tryptophan away from serotonin production and toward the creation of neurotoxic metabolites. This biological “hijacking” is a leading theory in why chronic digestive issues are so frequently comorbid with clinical depression.
5. The Kynurenine Pathway and the Biochemistry of "Brain Fog"
When the “Second Brain” is in a state of distress, it changes the way it processes amino acids. Under conditions of systemic inflammation or gut dysbiosis, the enzyme indoleamine 2,3-dioxygenase (IDO) is upregulated. This enzyme breaks down tryptophan into kynurenine, which can then cross into the brain and be converted into quinolinic acid. Quinolinic acid is a potent “excitotoxin” that overstimulates NMDA receptors in the brain, leading to the death of neurons and the sensation of “brain fog” or cognitive fatigue. This explains why people with poor gut health often report that they cannot “think straight”—their gut chemistry is literally producing a mild neurotoxin that interferes with clear neural transmission.
6. Microbial Cravings: The Science of Host Manipulation
The bacteria in your gut are not passive bystanders; they are active competitors for resources. Different species have different “optimal” fuel sources. For example, Prevotella thrives on carbohydrates, while Bacteroidetes favors certain fats. Research suggests that these microbes can manipulate host behavior to get the nutrients they need to outcompete other strains. They do this by changing the sensitivity of your taste receptors, making sugar or fat taste more rewarding, or by releasing “cravings signals” that mimic human hunger hormones like ghrelin. When you feel an uncontrollable urge for a donut, it may not be “you” wanting it, but a specific population of sugar-loving microbes demanding a refill of their preferred substrate.
7. The Role of GABA and the Biological "Mute Button"
Anxiety is often characterized by an inability to quiet the mind, a function regulated by the neurotransmitter GABA (Gamma-Aminobutyric Acid). Fascinatingly, specific strains of gut bacteria, such as Lactobacillus rhamnosus, have been shown to produce GABA or influence the expression of GABA receptors in the brain via the vagus nerve. In clinical trials, subjects who consumed these specific “psychobiotics” showed a measurable reduction in cortisol levels and a higher tolerance for stress. This suggests that a well-balanced microbiome acts as a biological “mute button,” helping the brain filter out unnecessary stress signals and maintain emotional homeostasis.
8. Intestinal Permeability: When the Barrier Breaks
The lining of the gut is a single layer of epithelial cells held together by “tight junctions.” These junctions act as the “security guards” of the body, deciding what gets into the bloodstream and what stays out. When these junctions are damaged by chronic stress, processed seed oils, or excessive alcohol, the gut becomes “leaky” (Intestinal Permeability). This allows Lipopolysaccharides (LPS)—the toxic outer shells of certain bacteria—to “leak” into the bloodstream. Once LPS enters systemic circulation, it triggers a massive immune response. Because the blood-brain barrier shares similar protein structures with the gut barrier, a “leaky gut” often leads to a “leaky brain,” allowing inflammatory markers to enter the central nervous system.
9. The Immune System’s Training Ground
Approximately 70% to 80% of the human immune system is located within the gut, specifically in the Gut-Associated Lymphoid Tissue (GALT). The microbiome acts as the primary “drill sergeant” for these immune cells. Through a process called “cross-talk,” bacteria teach immune cells how to distinguish between harmless food particles and dangerous pathogens. When microbial diversity is low (often due to over-sanitization or lack of dietary fiber), the immune system becomes “bored” and hyper-reactive, leading to the development of food sensitivities, allergies, and autoimmune conditions. A diverse gut isn’t just about digestion; it’s about maintaining an educated and precise immune defense.
10. Dopamine and the Reward Loop of the Gut
While serotonin handles the “peace” of the mind, Dopamine handles the “drive.” The gut-brain axis plays a critical role in the reward circuitry that governs motivation and addiction. Certain gut microbes are capable of synthesizing dopamine or its precursors. When we eat foods that support a healthy microbiome, the gut sends signals to the brain’s ventral tegmental area (VTA), releasing a steady, sustainable pulse of dopamine. Conversely, a dysbiotic gut can lead to “dopamine crashes,” leaving an individual feeling lethargic and unmotivated, and driving them toward “quick fixes” like caffeine or refined sugar to temporarily boost their mood.
11. Pros and Cons: A Detailed Comparison of Gut States
| Category | Symbiosis (Optimal Balance) | Dysbiosis (Imbalance) |
| Mood Profile | High resilience; stable serotonin levels. | Anxiety-prone; fluctuating mood; irritability. |
| Cognitive State | Sharp focus; high mental endurance. | “Brain fog”; forgetfulness; mental fatigue. |
| Cravings | Natural appetite for diverse whole foods. | Intense, urgent cravings for sugar and salt. |
| Sleep Quality | Deep REM sleep; high melatonin production. | Insomnia; restless sleep; night-time hunger. |
| Immune Function | Precise; low systemic inflammation. | Overactive; prone to allergies/inflammation. |
| Skin Health | Clear; resilient “gut-skin axis.” | Prone to acne, eczema, or redness. |
12. Circadian Rhythms: Does Your Gut Have a Clock?
Your “Second Brain” operates on its own circadian rhythm, independent of the light-dark cycle seen by your eyes. Gut bacteria fluctuate in population and activity levels depending on the time of day. When we engage in late-night eating or experience jet lag, we desynchronize our “head clock” from our “gut clock.” This “circadian misalignment” causes the microbiome to shift toward a more inflammatory profile. Studies have shown that simply restricting food intake to a 10-hour window (Time-Restricted Feeding) can significantly improve microbial diversity and metabolic health, even if the diet itself remains unchanged.
13. The Impact of Early Life and Birth Method
The foundation of the “Second Brain” is laid during the first 1,000 days of life. The method of birth (Vaginal vs. C-section) and the method of feeding (Breastmilk vs. Formula) determine the “founding species” of the microbiome. Infants born via C-section often lack the Bifidobacterium strains found in the birth canal, which are crucial for early immune education. While these gaps can be bridged later in life through diet and probiotics, the “seeding” process highlights how deeply our adult mental and physical health is rooted in our earliest microbial exposures.
14. Psychobiotics: The Future of Mental Health Treatment
The emerging field of “Psychobiotics” involves using specific bacterial strains as a therapeutic intervention for psychiatric disorders. Unlike traditional antidepressants that focus solely on brain chemistry, psychobiotics target the source of the neurochemical precursors in the gut. For instance, strains like Lactobacillus helveticus have shown promise in reducing the “rumination” (looping negative thoughts) associated with depression. This “bottom-up” approach to mental health represents a paradigm shift, moving medicine away from the skull and toward the digestive tract.
15. Frequently Asked Questions (Deep-Dive Edition)
Can stress cause permanent damage to the gut? Chronic stress releases cortisol, which increases gut permeability and reduces blood flow to the digestive tract. While the gut is highly regenerative, prolonged stress can lead to “chronic dysbiosis,” making it difficult to maintain beneficial bacterial colonies without lifestyle intervention.
How does fiber actually “feed” the brain? Fiber is fermented by gut bacteria into Butyrate. Butyrate travels to the brain and stimulates the production of Brain-Derived Neurotrophic Factor (BDNF), which acts like “Miracle-Gro” for neurons, helping you learn faster and protecting against age-related decline.
What is the “Post-Antibiotic” protocol? Antibiotics are “scorched earth” for the gut. To recover, one should focus on S. Boulardii (a beneficial yeast that survives antibiotics), followed by a massive increase in prebiotic fibers (onion, garlic, asparagus) to provide “real estate” for new beneficial bacteria to grow.
16. The Path Forward: Cultivating Your Inner Ecosystem
Understanding the “Second Brain” changes health from a battle of willpower into a practice of “internal farming.” To change your cravings and mood, you must change the environment in which your microbes live. This involves a three-pronged approach: Removing inflammatory triggers (processed sugars, chronic stress), Replacing missing enzymes or fibers, and Reinoculating the gut with fermented foods and high-quality probiotics. By treating your gut with the same respect as your brain, you unlock a level of mental clarity and emotional stability that was previously thought to be impossible.
Note: The science of the microbiome is rapidly evolving. Always consult a medical professional or a gastroenterologist before starting a new supplement or restrictive diet, especially if you have pre-existing conditions like IBD or SIBO.

17. The Holistic Integration: A Final Synthesis of the Bi-Directional Mind
The culmination of modern neuro-gastroenterology leads us to a singular, profound conclusion: the human experience is not localized solely within the skull, but is the result of a continuous, rhythmic dialogue between our two brains. We have historically operated under a “top-down” medical model, attempting to treat mood disorders, cognitive decline, and metabolic dysfunction by targeting the central nervous system in isolation. However, the staggering evidence regarding the Gut-Microbiome-Brain Axis demands a “bottom-up” revolution. To truly heal the mind, we must cultivate the garden of the gut. When we recognize that our cravings are microbial signals, our “brain fog” is often systemic inflammation, and our anxiety may be a distress call from the vagus nerve, we move away from the frustration of “lack of willpower” and into a state of biological empowerment. By prioritizing microbial diversity, protecting our intestinal barriers, and nourishing our enteric neurons, we do more than just improve digestion—we safeguard our mental clarity, emotional resilience, and long-term neurological health. The “Second Brain” is not merely a digestive assistant; it is the silent architect of our internal world, and the future of human wellness lies in our ability to listen to its subtle, chemical language.
Summary Table: The Gut-Brain Connection at a Glance
| Pillar of Health | Mechanism of Action | Long-term Impact of Optimization |
| Neurochemistry | Tryptophan/Serotonin conversion & GABA production. | Sustained emotional stability and reduced anxiety. |
| Structural Integrity | Maintenance of “Tight Junctions” (Zonulin control). | Prevention of neuroinflammation and systemic “leaky brain.” |
| Microbial Ecology | Competitive exclusion of sugar-seeking pathogens. | Elimination of intense cravings and metabolic crashes. |
| Neural Pathways | Vagus nerve signaling and afferent reporting. | Higher stress tolerance and improved “gut instinct.” |
Frequently Asked Questions
How do I know if my “Second Brain” is currently struggling? Common indicators of a disrupted gut-brain axis include persistent “brain fog” shortly after meals, a reliance on caffeine or sugar to maintain mood, chronic bloating, and an inability to handle minor stressors without a significant emotional reaction. If your digestion and your mood seem to fluctuate in tandem, it is a strong sign of dysbiosis.
Can exercise affect my gut-brain axis? Absolutely. Physical activity, particularly aerobic exercise, increases the diversity of the microbiome and promotes the growth of bacteria that produce Butyrate. This creates a “positive feedback loop” where exercise improves the gut, and a healthy gut provides the dopamine and energy levels required to maintain an exercise routine.
Is it possible to “over-fix” the gut with too many supplements? Yes. The goal is diversity and balance, not dominance of a single strain. Over-supplementing with a single probiotic can lead to “Small Intestinal Bacterial Overgrowth” (SIBO). The safest and most effective way to optimize the second brain is through a diverse, fiber-rich diet supplemented by fermented foods rather than relying solely on high-dose capsules.
Final Medical Disclaimer: The information provided in this article is for educational purposes and is based on emerging scientific research. It is not intended to diagnose, treat, or cure any medical or psychiatric condition. Because the gut-brain axis is highly individual, you should consult with a healthcare professional or a registered dietitian before making significant changes to your diet, especially if you have a history of eating disorders, autoimmune disease, or chronic gastrointestinal issues.